Hastalığın özyönetiminin önünde gözden kaçırdığımız engel: Sağlık inanışları
Genel bilgi: Diyabet, insulin hormonunun tam (tip 1 diyabet) ya da kısmi (tip 2 diyabet) yokluğu nedeniyle ortaya çıkan hiperglisemi ile karakterize kronik progresif bir metabolik bozukluktur. Tip 2 DM olan hastalarda, hastaya ait sonuçları iyileştirmek ve ölüm riskini azaltmakta tedavi uyumu çok önemli bir rol oynamaktadır.
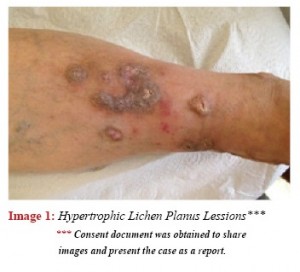
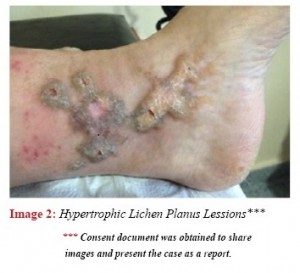
Vaka: 59 yaşında, 10 yıl önce tanısı konulan diyabeti ve hipertansiyonu olan kadın hasta, 6 gündür devam eden sol yan ağrısı şikayeti ile başvurdu. Fizik muayene bulguları: her iki ayakta hipertrofik lichen planus lezyonları, sol abdominal bölgede eri-tematöz veziküler punktiform lezyonlar, kan basıncı 150/70 mm Hg.
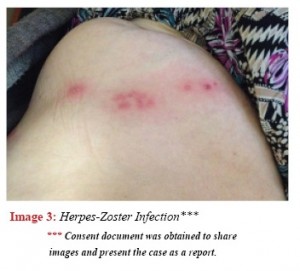
Laboratuar bulguları: HbA1c:13,3; Açlık kan şekeri: 329 mg/dl; idrar analizinde glukoz +++. Hastaya Herpes-Zoster enfeksiyonu tanısı konuldu; insülin tedavisi ve hipertrofik liken planus lezyonları ve Herpes-Zoster enfeksiyonu için tedavi düzenlendi. Buna rağmen, hasta insulin enjeksiyonlarını kullanmak istemediğini belirtti. Daha da önemlisi, ilk tanının üzerinden hayli zaman geçmiş olmasına rağmen, hasta hala neden böyle bir hastalığı olduğunu sorguluyordu.
Tartışma: Diyabet, spesifik tedavisi olmayan bir hastalıktır. Kısa ve uzun dönem komplikasyonların engellenmesi için hasta ve he-kim arasında devamlı işbirliğini gerektiren kronik ilerleyici bir durumdur. Bu nedenle tedaviye uyum, diyabet bakımında çok önemli rol oynamaktadır. Ancak ne yazık ki, hastalar sıklıkla tedavi rejimlerine uyum göstermezler.
Karar: Herpes-Zoster enfeksiyonu bizim için; hastanın sağlık algısını anlamak, etkili bir hasta hekim iletişimine başlamak, hastanın özgüvenini ve öz yeterliliğini geliştirmesine yardım etmek ve uygun bir kronik hastalık öz-yönetimine doğru adım atmak için bir fırsattı.
Tam Metin
Background
Chronic diseases are responsible for 60% of deaths annually (WHO, 2014).1 The number of individuals with chronic illness and multimorbidity is growing due to the rapid ageing of the population and the greater longevity of individuals.2 One of the biggest challen-ges for health care providers today is to address the continued needs and demands of individuals with chronic illnesses like diabetes. Diabetes Mellitus (DM) is a chronic progressive metabolic disorder characterized by hyperglycaemia mainly due to absolute (Type 1 DM) or relative (Type 2 DM) deficiency of insulin hormone. World Health Organization estimates that more than 346 million people worldwide have DM. This number is likely to more than double by 2030 without any intervention.3 DM virtually affects every system of the body mainly due to metabolic disturbances caused by hyperglycaemia. Treatment compliance plays important role to maximise patient outcomes and minimise the risk of death in patients with type 2 DM. A study done by Crucial et. al showed that clinic non-attendance and/or medication non-compliance were each independently associated with increased all-cause mortality in patients with insulin-treated type 2 DM.4
According to the Chronical Care Model, one of the essential elements of high quality chronic disease care is self-management, defined as “the individual’s ability to manage the symptoms, treatment, physical and psychosocial consequences and lifestyle changes inherent in living with a chronic condition”.1 The aim of this study is to emphasise the importance of self-management by presenting a case who had a problem with accepting the diagnosis of type 2 DM because of her health beliefs.
Case
A 59-year old female with type-2 DM and hypertension, diagnosed 10 years ago, admitted to our outpatient clinic. She had a six-day history of left lateral abdominal pain which exacerbated particularly at nights and erythema located in the same area. She also complained about one-year history of urinary incontinence. In past medical history, besides diabetes and hypertension, she was suffering from hyperlipidemia and had a cataract operation a year ago. She explained that, although she had to, she had not used insulin therapy for three months because of injection area pain and problem with her insurance. She got treatment for lichen planus at dermatology clinic eight years ago and since then, she didn’t attend to follow-up appointments.
In the physical examination blood pressure was measured as 150/70 mmHg; on both feet there were detected lesions defined as lichen planus. (Images 1&2)
There were also erythematous, vesicular, punctiform lesions on the left lateral abdominal region that did not spread to the counter-side. (Image 3)
There was no sign of lipodystrophy. Laboratory findings of the patient was as follows: HbA1c:13,3; Fasting blood glucose: 329 mg/dl; (+++) glucose in urinalysis. Clinical findings were considered as the signs of Herpes-Zoster infection. And after a detailed history urinary incontinence was considered as a neuropathic complication of diabetes that has been consulted with dermatology and endocrinology clinics. Insulin therapy, medications for hypertrophic lichen planus lesions and Herpes Zoster infection were arranged.
However; she expressed that she did not want to use insulin injections. More importantly, although many years had passed since the first diagnosis, she was still questioning why she had this illness. Suddenly, with tearful eyes, she said “although she does her missions against to God, she has these illnesses and is addicted to medications so she is an evil person and cannot be recovered any time.” She thought having DM as a punishment because of something she did wrong. If she was a good person, she wouldn’t have to use insulin injections four times in a day. In this first visit, we explained the pathogenesis of these chronic conditions simply, informed about the complications and encouraged her to use her medications. After two appointments, fasting blood glucose levels were regulated. However, she did not come to her follow-up visits.
Discussion
This case presentation elaborates a patient with severe complications of Type 2 DM who did not comply with treatment, life-style changes and follow-up appointments. Diabetes is a disease with no specific cure and a demanding self-management regimen. It is a progressive condition that requires continuous management as well as patient and provider collaboration in order to avoid both short-term and long-term life-threatening complications.
Therefore, medication adherence plays important role in the clinical care of diabetes. Although good glycaemic control can help to prevent complications, patients often do not comply with medication regimens. Non-compliance leads to burdens for patients and for healthcare systems by increasing morbidity and mortality, reducing quality of life, and raising healthcare costs.5 Various studies have been made on reasons of non-compliance. According to these studies; non-compliance can be due to factors that are patient-related, therapy-related or healthcare system-related.
> The patient-related factors can be demographic (age, gender, educational level and marital status) and psychological (patients’ beliefs and motivation towards the therapy, negative attitude, patient-prescriber relationship, understanding of health issues, and patient’s knowledge).
> The therapy-related factors include route of medication, duration of treatment, complexity of treatment, and the side effects of the medicines.
> The factors associated with the healthcare system include availability, accessibility, and the physician’s management skills.6 Insufficient communication including incomplete history taking, conflicting information, neglected disagreements, or a disturbed relationship between the patient and the physician may cause non-adherence or non-compliance. Researches showed that patients who understand more their disease, health and lifestyle have better experiences and health outcomes are more likely to be adherent or compliant to treatment and often use less health care resources; the effect is even more when these patients are empowered to and responsible for managing their health and disease.2
In addition; it is established that, when a person faces the diagnosis of a chronic disease, he/she can go through the stages for mourning of Kubler Ross (shock, denial, anger, bargaining, withdrawal – depression, acceptance). Lacroix and Assal also described two other stages named; obedience and pseudo-acceptance.7 If one of these stages is prolonged, the process of treatment adherence may delay as well. The patient mentioned above seems to be in pseudo-acceptance stage. She thought that if she was a good person and did her missions against to God properly as a good Muslim, she wouldn’t have these chronic diseases and be addicted to insulin.
While she was crying, she said “I accept to have all these diseases, because it’s my destiny, because the God wants like that. Even if I comply with doctors’ advices, I won’t be recovered any time.” Her perception of her health and disease caused non-compliance to treatment. In a study done by Demirtaş et al. defined that people with type 2 diabetes refer full responsibility of the disease to God in pseudo-acceptance stage. They rely on doctors in a passive way and do not take active role in management of their self-care.8
Non-compliance is not only limited to the failure of taking medication, but also to the failure of making lifestyle changes, undergo tests or keep appointments with physicians. In addition to this fact, the new definition of health by Huber et al.; “Health is no longer defined as a static situation but as the ability to adapt and to self-manage, in the face of social, physical, and emotional challenges” indicates self-management as an important and irreplaceable part of health and disease management. The most important skills for self-management are problem solving, decision making, resource utilization, and taking action. The basic principle underlying self-management is that behavioural change cannot succeed without the patient taking responsibility. In addition to skills of patients, another necessary ingredient for self-management is a good relationship between the patient and health care provider.2
Conclusion:
Further investigations are needed to discover reasons of treatment non-compliance in patients with type 2 DM, it will provide better self- management strategies for both patients and health care providers. While managing chronical conditions with a «person-centered approach» we can understand patients’ health beliefs, perceptions and fears.
Herpes-Zoster infection was an opportunity for us to understand patient’s health beliefs and to start an effective patient-physician communication, to help the patient establish self-confidence and self-efficacy and take a step towards appropriate self-management of chronical diseases.
Referanslar
- Lily C, Johnston S, Guilcher S, Irving H, Hogel M, Jaglal S. Impact of a chronic disease self-management program on healthcare utilization in eastern Ontario, Canada. PrevMed Rep 2015; 2: 586-90.
- Talboom-Kamp E, Verdijk N, Harmans L, Numans M, Chavannes N. An e-health platform to manage chronic disease in primary care: an innovative approach. Interact J Med Res 2016; 5(1): 5.
- Shrivastava SR, Shrivastava PS, Ramasamy J. Role of self-care in management of diabetes mellitus. J Diabetes Metab Disord 2013; 12(1): 12-4.
- Currie J.C, Peyrot M, Morgan C.L, et al. The impact of treatment noncompliance on mortality in people with type 2 diabetes. Diabetes Care 2012; 35(6): 1279-84.
- Brundisini F, Vanstone M, Hulan D, DeJean D, Giacomini M. Type 2 diabetes patients’ and providers’ differing perspectives on medication nonadherence: a qualitative meta-synthesis. BMC Health Serv Res 2015; 15:516; 1174-8.
- Khan A.R, Lateef A.Z.N, Al Aithan M.A, Bu-Khamseen M.A, Al Ibrahim I, Khan A.S. Factors contributing to non-compliance among diabetics attending primary health centers in the Al Hasa district of Saudi Arabia. J Family Community Med 2012; 19(1): 26-32.
- Ismail K, Winkley K, Rabe-Hesketh S. Systematic review and meta-analysis of randomised controlled trials of psychological interventions to improve glycaemic control in patients with type 2 diabetes. Lancet 2004; 15;363(9421): 1589-97.
- Demirtaş A, Akbayrak N. Tip 2 diabetes mellituslu hastaların hastalıklarına uyum ve kabullenme kriterlerinin belirlenmesi. Anatol J Clin Investig 2009; 3(1);10-18.